Amongst healthy adolescents, there is a near-normal distribution of the timing of puberty, with the mean age of onset in boys being 11.5 years and in girls 11 years, but wide inter-individual variation (age range 9–14 years in boys; 8–13 years in girls) (1). The timing of puberty is strongly heritable, and evidence from twin and other epidemiological studies has demonstrated that genetic regulation is an important element in determining when healthy individuals enter puberty. Such studies suggest that 50–80% of this variation in the general population is under genetic regulation. However, an individual’s nutritional status, adoption, geographical location and emotional well-being also have an effect on pubertal timing.
Amongst healthy adolescents, there is a near-normal distribution of the timing of puberty, with the mean age of onset in boys being 11.5 years and in girls 11 years, but wide inter-individual variation (age range 9–14 years in boys; 8–13 years in girls) (1). The timing of puberty is strongly heritable, and evidence from twin and other epidemiological studies has demonstrated that genetic regulation is an important element in determining when healthy individuals enter puberty. Such studies suggest that 50–80% of this variation in the general population is under genetic regulation. However, an individual’s nutritional status, adoption, geographical location and emotional well-being also have an effect on pubertal timing.
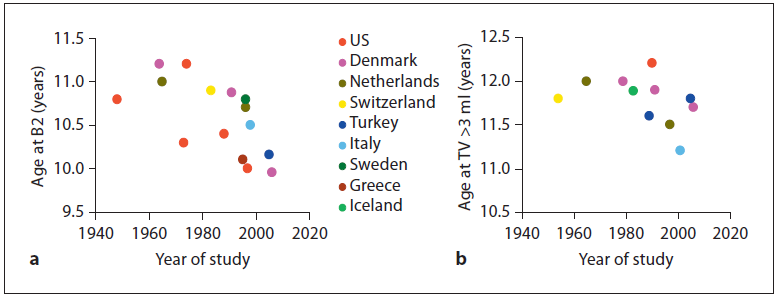
The timing of puberty in most developed countries exhibited a rapid decrease in the first half of the 20th century. This was most notable in girls (Figure 1, panel A), but has also been documented in boys (Figure 1, panel B). This has resulted in an increase in both the number of cases of central precocious puberty and in the incidence of normal variants of puberty (premature thelarche and adrenarche) (1). This observed secular trend towards an earlier age of pubertal onset has been the subject of intense discussion. In view of the timeframe, it is thought not to be genetically determined, but likely due to increasing rates of obesity in children and other environmental influences.
There are clear data supporting the influence of nutritional changes on pubertal timing, as shown by the clear correlation between age at puberty onset and childhood body size, particularly in girls. A larger gain in body mass index (BMI), particularly between 2 and 8 years of age, is positively associated with first breast development (2) and fat mass percentage during a similar period in mid-childhood has been shown to be associated with increased risk of precocious puberty in boys (3). In boys, the data suggest a complex relationship between fat mass and pubertal timing, with overweight status associated with earlier pubertal onset but severe obesity correlated with later onset (4), potentially due to suppression of the hypothalamic–pituitary–gonadal (HPG) axis.
In conclusion, the observed increase in the incidence of both central precocious puberty and benign pubertal variants is most likely due to increasing BMI of children in the developed world and a possible influence of EDCs. This has clinical significance as earlier pubertal development has associations with poor adult health, including risk of type 2 diabetes, cardiovascular disease and breast cancer, as well as psychosocial difficulties in adolescence and beyond (1).